Prediction of gender using conduction intervals and axis from 12-lead ECG
Introduction
Artificial intelligence has been used to identify abnormal patterns in electrocardiograms and assist clinicians in making medical diagnoses. These systems have been trained to replicate a human understanding of data and patterns. Neural networks have been developed to exceed the capabilities of board-certified cardiologists in arrhythmia identification from single-lead rhythm strips.
Cardiologist-Level Arrhythmia Detection with Convolutional Neural Networks (Rajpurkar et al.)
In this study, I explore the capability of neural networks to extract meaningful information from a 12-lead ECG beyond what a human clinician is capable of perceiving. Specifically, I investigated the use of a neural network to detect the gender of a patient from the conduction intervals and axis data from the ECG — parameters that any trained physician could access but could not reliably use to determine gender.
Methods
The conduction intervals and axis data were extracted from 93,740 de-identified 12-lead ECGs obtained through the Philips DXL ECG Algorithm in an automated process. The following data points were collected:
- → RR interval (heart rate)
- → PR interval
- → QRS duration
- → QT and QTc intervals
- → P wave axis, QRS axis, T wave axis
ECGs with missing values were excluded. Patients in atrial fibrillation or flutter were excluded (no measurable PR interval). The age of the patient was manually entered by the technician at the time of the tracing. Gender was recorded as reported by the patient.
Data normalization was applied using min-max scaling:
Axes were standardized to positive values — for example, an axis of −45° was encoded as 315°.
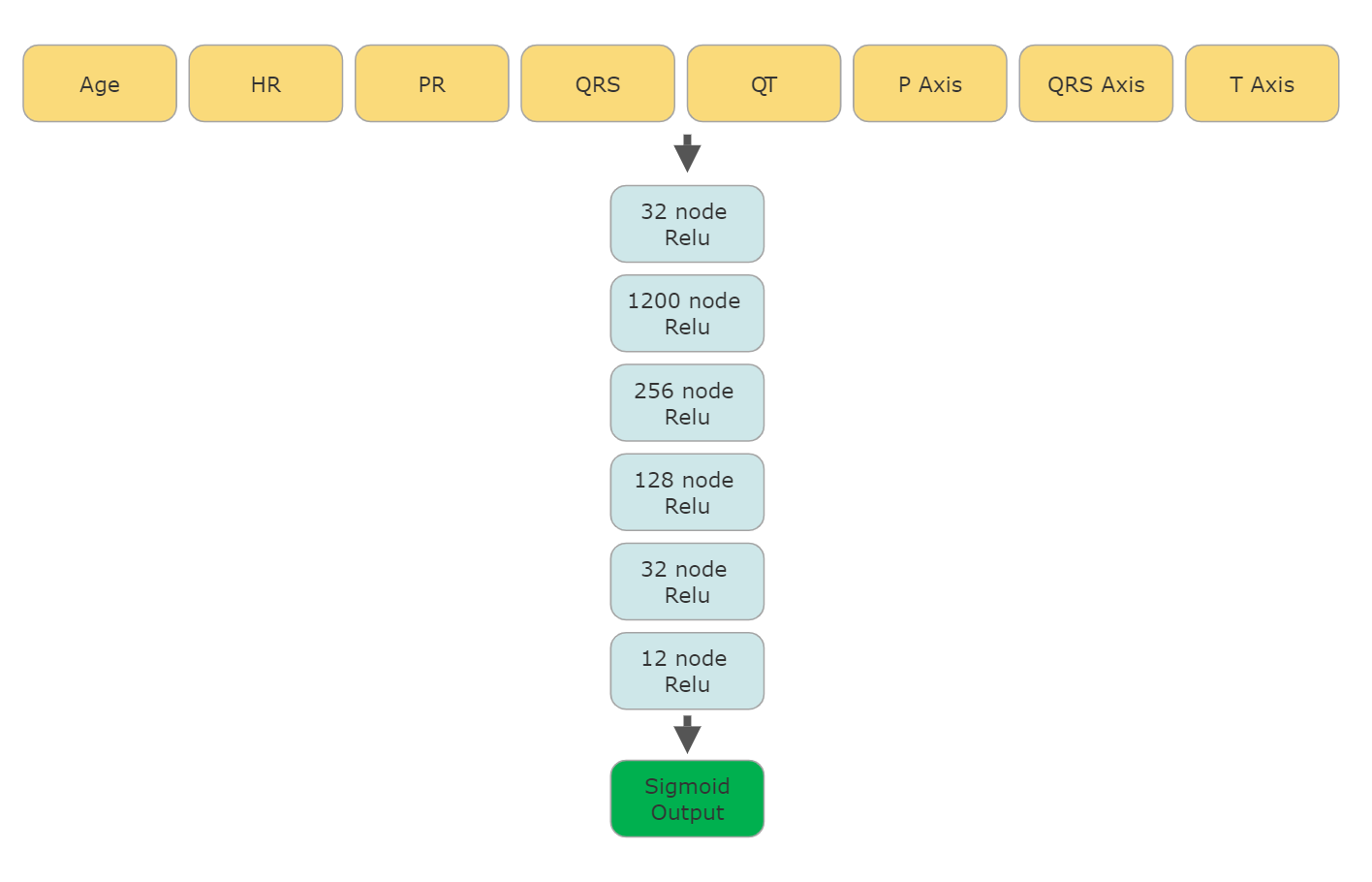
Results
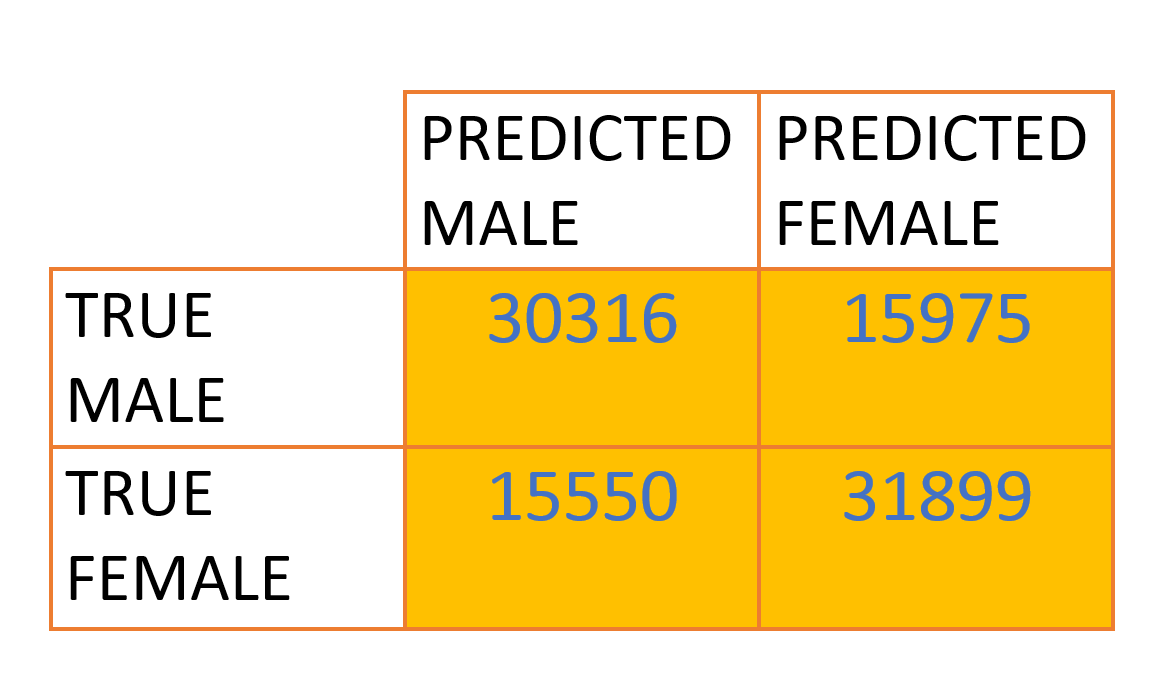
Overall accuracy in predicting patient gender from ECG conduction intervals and axis — significantly better than the 50% chance level of a random guess.
The neural network achieved 66.4% overall accuracy in predicting patient gender from conduction intervals and axis data alone. While this is a modest absolute number, it is meaningfully better than the 50% baseline that a clinician can offer when asked to predict gender from the same parameters.
The receiver-operator curve (ROC) demonstrates the model's discriminatory ability across different classification thresholds, confirming performance above chance in a dataset of nearly 100,000 ECGs.
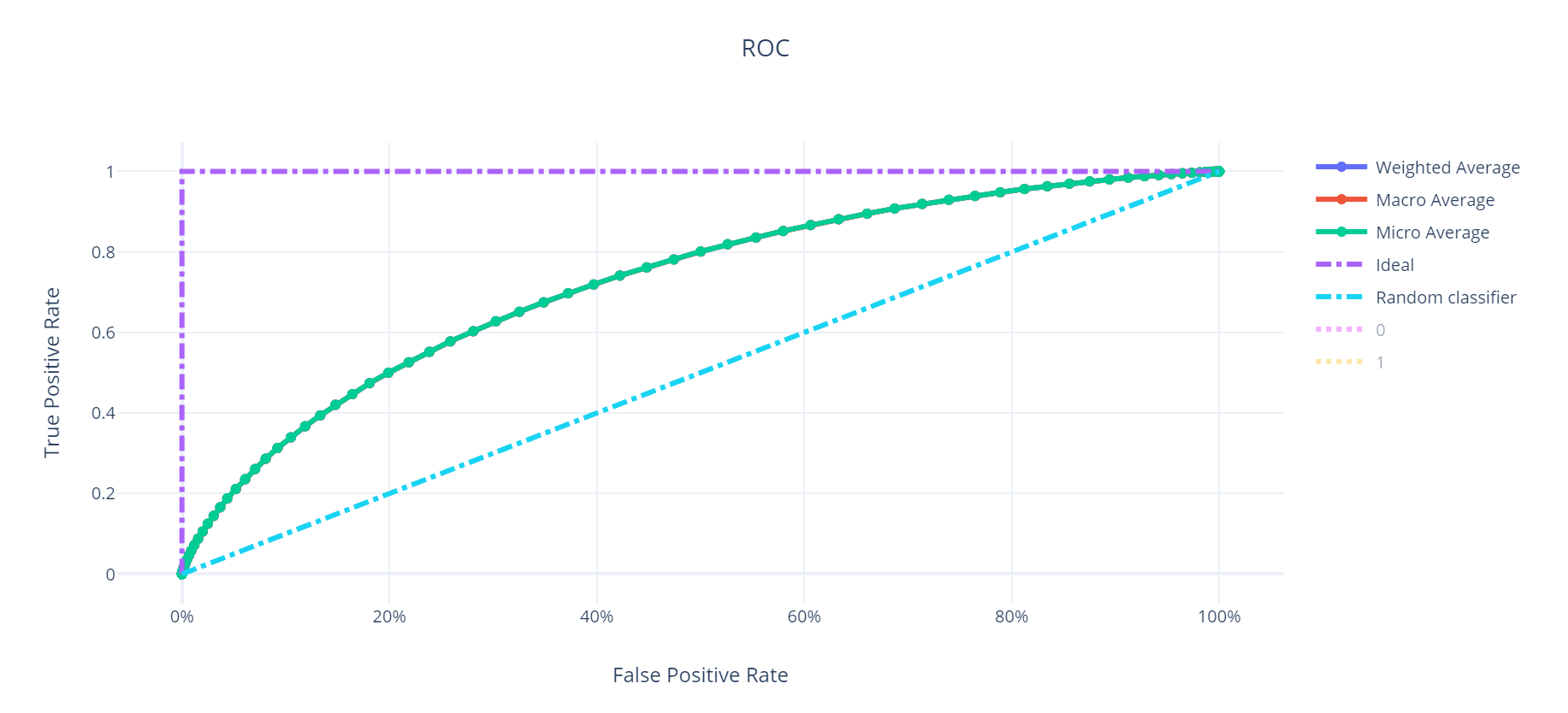
Discussion
The findings from this study show that gender is predictable from simple parameters of a 12-lead ECG to a degree that exceeds human perception. A trained physician cannot reliably predict a patient's gender based on the same data that the neural network analyzed.
This suggests that ECGs — and many other routine diagnostic tests — may contain more clinically useful information than is apparent to clinicians. The use of artificial neural networks may improve the diagnostic yield of commonly available tests and reduce the need for extensive additional testing.
More broadly, this study illustrates a key premise about AI in medicine: neural networks may detect patterns in data that are genuinely super-human — not by replicating clinical reasoning, but by identifying statistical relationships that are invisible to the trained human eye.
Key Implication
Diagnostic tests may contain useful information that is not apparent to clinicians. Neural networks offer a path to extracting that hidden information — potentially reducing redundant testing and improving diagnostic efficiency at scale.
